
It’s been a long time since I’ve written about anything other than wine, but I have found in preparing for my own total hip replacement, there is a lot of conflicting information and misconceptions – especially for fairly (ahem) young people who have, and wish to continue, leading an active lifestyle.
I remember after my knee reconstruction feeling very alone and wishing that I could pick someone’s brain who had walked the same path as me. Fast forward 5 years and I am now preparing for total hip replacement at 53, and I’ve decided to chronical my experience on the chance that it might help someone else.
THE SITUATION
I’ve had trouble with my hip for many years, although it is hard to pinpoint when it first started. I suspect it began in 2013 when I fell playing tennis. I was sore all over, but the focus of that fall was my knee which I felt like I had completely blown out. It turns out I did, but I wouldn’t confirm this fact for nearly three years.
I continue a very active lifestyle despite not having an ACL – ignorance is bliss as they say. I actually end up in the best shape of my life during this time due to weight lifting. I do not ever return to kickboxing or tennis – quick lateral movements are not something I can do. In hindsight, because my Mom was battling Stage IV cancer like a boss, I probably thought that a wonky knee was not even a real problem.
I think it is during this time, that I do recall having incredible hip pain when I go from sitting to standing and first start walking, but I think this is related to the tennis fall and my wonky knee – even though it is on the other side. I start Yin yoga during this time, which changes my life for many reasons, but in hindsight, I think Yin yoga plays a huge factor in my ability to get around pain free for the most part.
In September of 2016, on the first day of my vacation in Italy, I create a bucket handle meniscus tear in my left knee. This happens in my hotel room, while sitting on the bed, with a minor move of my bum off of my knees. With this type of tear, it is not possible to straighten my knee. Long story short, I fly home in a wheelchair. I make lots of friends that are far more “mature” than I am and they help me put things in perspective, but I cannot lie. This is my first trip to Italy, it is for our 25th wedding anniversary and this is a jagged little pill to swallow, especially if you know my wedding story. I seriously wonder if my marriage is cursed, but I need someone to push my wheelchair so I try not to think about it.
Following an MRI for this injury, I discover that I have the bucket handle meniscus tear and also that I have no ACL. They ask me when I tore my ACL because it is clear that it is an old injury. Once this diagnosis is made, I actually have surgery within just a few days. What was supposed to be a fairly simple surgery, with just two arthroscopic entry points, turns into flaying my knee wide open and post op instructions of no weight bearing for 6 weeks due to the meniscus repair (instead of menisectomy). I also have to rehab that new ACL. I don’t get cleared from my surgeon for nearly 9 months. It is 8 before I can return to yoga. I include all of this information because I am certain that the compensating my body did for not having that ACL, and then rehabbing for such a long a period of time, did not help my hip at all.
My personal life is fairly frantic and traumatic from 2011-2018. My Mom is battling Stage IV cancer, I am running back forth to Ohio, working, having kids graduate from high school, go to college, graduate from college, etc. I don’t have time to deal with my hip and a fairly regular yoga practice, chiropractic care and massage keep me pretty mobile, but I have gone from having a wonky knee to having a bad hip.
THE WRITING ON THE WALL

In early 2020, during the original Covid “lockdowns,” I am on 3.5 miles with my daughter and about half way in, I am in so much I am having to stop. Doing a quad stretch – pulling my heel to my glute gives me some relief but I am limping all the way home. That same week I go out to walk again and get to the end of my driveway and decide not to walk. The pain in my hip is excruciating.
I had not been seeing the chiropractor regularly so I start going twice a week and it truly does help. I also start taking a glucosamine/chondroitin from Costco. I’ve never experienced such a noticeable difference from a supplement before. In hindsight that quad stretch helped so much because I would find out that my hip was bone on bone and pulling the top of the femur away from the socket gave me some relief. Crazy.
I think I’m doing pretty good through 2020 and 2021. It is on my list of things to do to find an orthopedic for my hips which I’m still assuming is a misalignment, or muscular in nature and that a few weeks of PT will help. I end up having an unrelated abdominal CT scan in August of 2020 that reveals “severe osteoarthritis” with gluteus maximus and minimus muscle atrophy in my right hip. The muscle atrophy really bothers me. My Dad is sick during 2020 and actually passes away in August. My hip is not hurting as much as my heart and I put this on the backburner. My daughter gets engaged in December of 2020 and married in August of 2021, I’ve got plenty to distract me, but I resolve to get this hip looked at after the wedding.
In September of 2021, I had another abdominal CT scan – again for a completely unrelated issue – and it showed degenerative changes to my right hip from the previous year – also my spine. By this time I was also aware that I was starting to live a life that always took in to consideration my hip. Depending on the day, I would avoid errands that required me to walk a long a way or carry anything heavy or large. I was walking less. I was still going to yoga but I knew my hip was getting worse not better. It was time.
THE CONSULTATIONS

I started with a doctor who is very well known. When I called to make the appointment, I was reminded that I had initially made an appointment with this doctor for me knee back in 2016. He is in such high demand that by the time the appointment rolled around, through some divine intervention, I was already recovering from my knee reconstruction surgery with another doctor. This time, when I called about my hip, he had a cancellation and I was able to see him within a few days. Three things stood out for me at this appointment:
- I had a bone on bone hip and I needed a total hip replacement
- According to my doctor, this was an easy surgery – especially compared to knee reconstruction. He said I would be walking out of the surgical center, same day.
- The doctor said my x-rays did not match my range of motion and ability to walk without a limp. He was shocked. That made two of us.
This doctor said we could try a cortisone injection, but he didn’t have high hopes for the success of it because of the advanced stage of my hip. This guy has been doing this for decades though and he said you just never know and if I wasn’t ready for surgery we could certainly try it.
I was so surprised that I needed a hip replacement, I didn’t really ask the right questions. I left there without the information to make a decision, but of course, I started googling and picking the brain of anyone who had experience with total hip replacement surgery.
I would soon come to find out that there are two different approaches and that most people think the difference between the two are like night and day. People seemed very, very passionate about their opinions on which surgical approach to take – even people who have never had hip replacement surgery. I might as well have been asking if I should be a Democrat or a Republican – people were that rabid about their thoughts on this.
I speak with the doctor’s nurse to ask all of the questions I didn’t know to ask at the initial appointment, and I am informed that he only performs the posterior approach surgery. I’m surprised by this because I’ve talked to a couple of people who have had this surgery with him and they all attest it was the easiest surgery they’ve ever had – including an 80 year old woman who lives alone and was doing her own laundry on Day 3 post op. Regardless, I decide I at least need to have a consultation with a doctor that does the anterior approach so that I can make the best decision for me. This may be an easy surgery, but it is still a major surgery and I need to know everything before I decide.
I call a doctor who performs anterior and who comes highly recommended from several people. I call at around 10:00, knowing that I probably won’t be able to get in to see him for several weeks. They inform me they have a cancellation at 1:00. Are you kidding me? Is this some sort of sign? I tell this doctor that this is a second opinion, I tell him who I’ve seen already and that I really liked him, I just want to make an informed decision. The first thing he tells me is that I’ve probably read anterior is “non-invasive” and the recovery is easier, which is true, this is what I’ve read and heard. He makes it very clear that this is a fallacy and I need to get it out of my head. This is an invasive surgery, it does not matter where they enter my hip from. And the recovery time is the same, it is just different. He tells me that in the last 5 years the two procedures have both come such a long way that there is truly very little difference between the two. This is what the other doctor’s office said as well. At this appointment, the following sticks with me:
- I do in fact have a bone on bone situation, in fact this doctor calls it “end stage” osteoarthritis. That’s annoying. I’m not dying. He tells me cortisone injections are not an option.
- Regardless of approach – this doctor does both – the incisions are about the same length and only about 6 inches apart. Very contrary to everything I’ve heard and read. He says I am an excellent candidate for anterior but the decision is mine to make.
- This doctor is much more serious in his approach, it is both comforting and concerning.
I leave this office with an appointment for an anterior surgery date in January. I’m not at all committed to this, I’m still trying to get on the other doctor’s schedule at this time as well. My plan is to ask a few more questions to the first doctor, but I’m fairly certain since both doctors tell me there is no difference at 8 weeks with either surgery that I am going with the first guy, I have no reason not to, I liked him a lot and I have several people who have had surgery with him telling me to not give it a second thought.
Unfortunately, I l learn that getting a hold of doctor #1’s scheduler is a feat all by itself. I have someone who’s husband is having hip replacement with him and she shares the scheduler’s extension number and her email address. I make some progress but we are still playing phone tag as Thanksgiving comes and goes. The holidays are here and I am getting more confused by the day. I have a friend who just had hip replacement with Dr. #2 – she had posterior but absolutely loves the experience and the results. Dr. #2 requires a surgical clearance from my primary care and that appointment is fast approaching, as is my PreOp visit with Dr. #2’s PA. I am stressed beyond belief trying to make a decision.
I go to the surgical clearance appointment, and I go to my PreOp appointment with Dr. #2. I tell the PA, I am still not sure about my decision and I ask him what he would do. He says he is a runner so he would have hip resurfacing. I ask why that hasn’t been presented as an option for me, and he tells me it only works on larger joints and is generally not an option for women, certainly not 5’3″ women. I feel some relief that I can at least rule something out. He tells me Dr. #1 has a couple of decades on Dr. #2, but that the two them are probably the busiest hip replacement surgeons in the area and that if he couldn’t choose resurfacing, he would probably go with anterior.
I’m emotionally exhausted. Only I could consult with the two top surgeons in my area for this procedure, get to seem both of them quickly based on cancellations, and be completely paralyzed by indecision. I make the decision at this appointment that I’m gong with Dr. #2. I think I am in excellent hands either way and I just need to decide. I put it in God’s hands – because in reality that’s the only person who’s hands I’m in. Done. In less than one month, I will get a new hip. Anterior approach.
Try as I might I can’t wrap my head completely around my decision to even have this surgery. I have good days and I seriously question if I am doing the right thing. Against my better judgment I am still trolling the internet on searches of “yoga after hip replacement” and “golf after hip replacement.” Of course, this is counterproductive. Just stop it Cathie. Give it to God.
COVID SURGES, surgery prep and ONE MAJOR MELTDOWN
As Christmas approaches, we are in the largest Covid surge we’ve seen so far. The US is posting 1M cases a day, four times the peak amounts of 2020. My daughter and son-in-law are here from Wyoming and they are staying for three weeks. This proves to be a great distraction for me, but they are of course visiting friends and his family. We have a Covid scare the first week of January but all tests taken are negative.
The weather is warm in Atlanta and my husband and I decide to put my new golf lessons and clubs to the test on an actual course. We find a short course that is suited for a beginner. We golf 14 holes before the sun sets. I am in a pretty severe pain by the end and it’s not just my hip. It is my back and my shoulders. Because I am becoming less and less active due to my hip, my entire body is suffering. I am weak. I have no stamina. I am not getting any younger and I am reminded this is going to go down hill fast if I don’t get my hip fixed and get back to being in better shape.
While speaking to the insurance and billing person one week out, she casually mentions that my husband will have to leave me at the door. This is due to Covid she says. This is contradictory to the information the Surgical Coordinator sent.
ME: “But wait, you haven’t asked me to get a test prior to my procedure? Did you forget?”
HER: ‘No, if you are vaccinated, we do not require a test prior to procedure.”
ME: “So, let me get this straight. You are so worried about Covid that I cannot have a loved one with me while I wait 1-2 hours in PreOp, but you are not requiring me to get tested because I’m vaccinated?”
This makes absolutely no sense. I’m not going to lie, I lose my shit. I don’t want to be in the care of people who make such stupid decisions. Everyone who has this version of Covid is vaccinated! I had Covid in August and I am vaccinated. Vaccination means absolutely nothing in terms of whether or not I have Covid, but hey let’s not worry about that. We are, however, going to separate you from your loved one with no link to the outside world – I am asked not bring valuables including my phone – can’t be responsible for valuables.
I call my doctor’s office and cancel my surgery. I can wait. Even another year. I’m just not doing this, it is elective, and I elect to wait until I can put my life in the hands of people who make decisions that make sense to me. And that I don’t have to worry about being robbed from.
To my surprise both the doctor’s nurse and the surgical center coordinator validate that this makes no sense. Neither of them can say very much of course, but the fact that they agree it makes no sense makes me feel somewhat better. The nurse also points out that she has lost any hope that things will ever make any sense – especially in the medical care community. She is a seasoned professional who has been at this a long time. She tells me that they are not going to fill that spot, so just think about for a little bit longer. She hates that I’ve gotten through all of the preop appointments, etc. and things could get worse before they get better. The surgical center coordinator promises to meet me at PreOp and stay with me the entire time. I don’t know her, so as sweet as this, I’d probably rather not have a stranger pretending to be my loved one – that’s just weird. But I do appreciate the sentiment.
My husband expresses his annoyance at my cancelling. I am annoyed that this is nothing more than an inconvenience to his schedule. Suddenly, I realize I don’t really need him with me anyway lol! I sleep on this. The more I think about it, I am actually happy to have this done while they are not requiring a Covid test from me because at least the stress of worrying about the results is not something I have to deal with. God’s got this, I don’t need my husband with me in PreOp. I wake up with the decision that the world just doesn’t make sense right now. Take it or leave it. I don’t want to live my life anymore with the idea that it will be better “after I get my hip fixed.”
I get a text from my son in law’s mom, Karen. She says she is praying for everyone on my care team but reminds me I’m in God’s hands, and those are the best hands. I used nearly the exact same language to justify going ahead with this surgery and it feels like a divine sign from above. A God wink. Game on.
DAY OF SURGERY
I am the first surgery of the day. I am asked to arrive at 6:00 but warned that the surgical center doors don’t open until 6:00. They try to check me in in the hallway and send my husband on his way but they have the amount of money left to collect incorrect. I’m not sure why this wasn’t all handled prior to today but, nevertheless, they send me in to the office to get the correct amount taken care of and make my husband wait outside. I only grabbed the FSA card from him in the hallway and it doesn’t allow the amount needed. She tells me she can bill me, but I don’t like that idea so I ask her if I can go grab my husband who I’m sure hasn’t gone anywhere just yet and get a credit card. She’s says that is entirely up to me. I find my husband in the lobby of the building, grab his credit card, take it back to the office, pay, and then return it to him in the hallway. I am trying to stay calm but this feels chaotic. I have to remind myself, I chose to do this. God’s got this. Just breathe.
I am taken back to PreOp and things move very quickly. It is the first time I have ever experienced being completely knocked out in PreOp. The last thing I remember is the anesthesiology coming to give me the nerve block, and the nurse telling me that she was giving me something to help me relax. I am knocked out within seconds. I have no recollection of being moved to the OR, of being transferred to the OR table. I’m just going to come right out and say it, this doesn’t feel good. I have never experienced not being knocked out in the OR with my surgeon present.
I wake up in PostOp and my husband is allowed in after they get me dressed. They accidentally remove my IV before giving me an antibiotic and they have to put a new one in near my elbow. I get the impression that it is a contest to see how fast they can get me out of here and that IV mistake is a direct result of being in a hurry. We go over the discharge instructions that they made me sign prior to surgery. I walk across the room, up and down and couple of steps and I am discharged. We are home by 11:00 a.m. Again, I remind myself that I chose to do this.
I follow the instructions and get up and walk every hour that I am awake. My mind is completely blown that I have had a portion of my femur sawed off, a hole drilled, and a metal rod placed in it and I am walking laps in my house with no pain. I know it is because of the nerve block but still, it’s pretty mind blowing. I take the required low dose aspirin and the Tylenol 650 mg as instructed and sleep well.
DAYS 1-3 POSTOP
Thursday continues with the walking every hour and by afternoon my thigh is incredibly sore. No hip pain at all but the thigh is pretty ouchy. I am using the walker and the worst pain is when I first stand, once moving it feels better. Tonight I take a Percocet before bed and sleep really well. On Friday, I wake up feeling really good with noticeably less thigh pain.
I have a PT appointment on Friday morning. They check my incision dressing and that’s about it. We don’t go over the exercises I’m supposed to be doing, nothing PT related. My pre-operative appointment was a little more informative but not much. Again, if it’s Covid we are all concerned with, both of these could have been handle with a Teledoc appointment with absolutely no difference in outcome. I’m doing the exercises on the handout they sent me home with and I’m walking every hour. In addition to the walking and low dose aspirin, I’m sleeping with a device that gently squeezes my calves – they take blood clots very seriously these days.
On Saturday my thigh pain is again improved and I switch from the walker to a cane. The stairs are definitely easy to manage and I’m having no issues getting around the house. I am having issues sitting and/or lying in the same position. I’m also fairly certain that my surgical leg is noticeably longer than the other leg. I had mentioned this at my PT appointment and was told that sometimes happens. I’m disappointed in this and hoping it improves somewhat over time. My thigh definitely hurts more by the end of each day but overall I am gaining noticeable improvement by the day.
My hip doesn’t hurt but since I have limited range of motion its hard to know if this is because of my shiny new hip joint, or if its because I am limiting my ROM. Let’s hope its because of my new hip joint.
DAYS 4-6 POST OP
My biggest challenge is sleeping on my back and sitting with my legs mostly straight. My low back/hip hurts and its because I just really need to do a forward fold or downward facing dog. I want to sit with my legs criss-cross applesauce. I begin googling PT moves for anterior hip replacement and learn that I can in fact foward fold to my comfort level. I can move my knee out to the side while bent. These things help.
It snowed on Sunday so I feel trapped even though I wouldn’t have left the house anyway. Ugh. I take Tylenol 650 mg at bed time just because my thigh is really sore at night.
On Monday, my husband brings out the slow cooker at my request and I chop veggies and assemble a vegetarian chili. I am moving around the counter area in my kitchen unassisted. Definitely not ready to completely ditch the cane, but I’m using it less. My thigh is still sore, and it’s still more noticeable as the day goes on and immediately upon standing.
My bandage is giving me anxiety. I want to take it off but need to wait a few more days. I also don’t want to take it off. I can see the Sharpie marks made by my surgeon and the anesthesiologist and I can see a big bruise. The bandage is huge – about 8″. I’m sure my incision is not that huge. But maybe it is? The leg length discrepancy is giving me anxiety. I made this decision that there is no going back from – this is giving me anxiety. Ugh. I’m trying to focus on the good things but I have been having noticeable heart palpitations and a general sense of panic.
By Day 6 I have researched the shit out of leg length discrepancies post THA. The information is hopeful. It is likely that I have an unnatural pelvic tilt forward due to the advanced stage of my arthritis. This will likely correct as I heal and the length discrepancy will feel less noticeable. I sure hope so. Today my glute muscle and hip feel sore but I’ve been pushing the rehab exercises pretty hard. I can put socks on by myself. This feels like a win.
DAYS 7-14 POST OP
Wednesday is the one week mark. The improvements have slowed a bit but still getting better by the day. My biggest complaint is this feeling of muscle tension/fatigue in my glute – it is hard to get comfortable sitting or lying. If I’m standing, bending the surgical leg knee so that my legs feel the same length helps. This leg length thing has me pretty wigged out.
It is 58 and sunny on Thursday, and my husband takes me on a short walk in the neighborhood. I am slow and I am limping far more than I ever did prior to surgery. I hope this is because I am far from healed. I am scared that it is due to the difference in leg lengths that seems to be becoming more and more of a problem for me. I hope I’m just being neurotic. Going outside made me realize how far I have to go in recovery. I can walk unassisted but I am super slow. I put on super baggy boyfriend jeans and real shoes today, it feels good. I’m not much a sweatpants girl to begin with, and a full week of PJs or sweatpants has me feeling bleck!
By the end of Thursday, this turns out to be my worst day. I’m in pain and it’s not just the thigh pain, I’m getting a pinching when I stand and put weight on my leg. My brain goes down a terrible bunny hole today. Maybe I will be in the small percentage of patients that don’t have a successful outcome. Maybe I chose the wrong surgeon. Maybe this, maybe that. Ugh!
Friday we take my Aquacell bandage off after dinner. They said 10 days and this is 10 if you count the day of surgery, but 9 if you don’t. Apparently I have an issue with adhesive that I did not know about – I have the reddest, itchiest rash everywhere the bandage adhesive touch my skin. I am somewhat relieved that taking the bandage off has improved the pinching feeling I was getting when standing and walking. I think perhaps the bandage was holding my hip in a position that was causing this. Crazy. The steri-strips/tape stay on and are nowhere near starting to fall off, so I still can’t really see this incision. This is fine with me – one thing at a time.
It was decided at my PreOp appointment that we would forgo the Celebrex due to my diverticulitis history. I feel completely fine in the GI department but I did spend the entire month of September with a case of “smoldering” diverticulitis and I really do not want to repeat this. Another flare up and I am more than likely going to have to have surgery to remedy this situation. Today, I decide to take Ibuprofen because I think I need an anti-inflammatory. My hip is feeling crappy enough that I decide it is worth the risk. I also rest my leg completely today, no PT exercises and no walking for the sake of walking.
On Saturday I wake up feeling so much better. It could be coincidence, but this seems to be the turning point for me. It’s hard to say that all of the discomfort I was feeling was in fact pain. It was also stiffness and a feeling of having inflammation going on – hard to describe and I apologize for that. I decide Ibuprofen is here to stay and I take it prophylactically on Saturday. I go with my husband to ride along on a couple of errands and I go in to one of the stores myself. When we get home, it is mid 50’s and sunny and I tell him I want to go for a walk. This goes much better, I am walking better and my hip feels really good. I feel so much better.
I wake up feeling more improvement on Sunday. I start – very carefully and intentionally – going up and down stairs normally but not without holding on to the rails tightly. I’m not really putting full weight bearing on my surgical leg when going up or down. I am slightly sore from my walk yesterday, but in a good way. I continue with the PT and walking. The rash is driving me crazy. I try Micellar water, alcohol, and nail polish remover to make sure that all of the adhesive is actually off of me. I am putting quite a lot of cortisone cream on the rash only. The steri-strips/tapes are still solidly in place.
Monday is a backwards day. I wake up with my leg not feeling as great as the day before and it goes downhill all day. I do some PT exercises early in the day, but not all of them. I should note that today the pain is definitely muscular – my glute is killing me and so is my inner thigh/groin. It doesn’t help that all of the inactivity is definitely showing up everywhere else on my body – I feel like a tightly wound spring.
My rash doesn’t look any better, still really red in the outline of my bandage, and extremely bumpy. I am wondering if there is somehow still adhesive on there? I carefully use olive oil and lightly massage into the rash while I’m having coffee, then I shower. The steri- strips/tape are not making much progress in coming off so I let them get a little wetter than I normally do and lightly use a scrunchy over the rash to get the olive oil off. So far I’ve just been using cortisone cream but a friend says she is allergic to adhesive and has had this situation often – she recommends Polysporin. My local drugstores do not have any in stock so my hubby orders on Amazon for next day delivery. All in all, its a crappy day and I am definitely not feeling better than before my surgery, which of course makes me question my decision. Overall, a not a great day.
Tuesday is the best day I’ve had since surgery and while my rash still looks awful it has miraculously stopped itching. I take a walk with my neighbor who is recovering from a serious fall and together we are the old ladies you see gingerly walking down the street. We are incredibly slow and I have my cane, we are quite the sight I’m sure, but it is sunny and 60 degrees and it is wonderful to be walking outside. We walked only about .15 or a mile and I am so surprised at how sore it makes me by the end of the day, but it is definitely muscle sore and not pain. Some of the steri-strips/tape are finally starting to come off and I can see part of the incision. I am terrible with incisions, stitches, staples, anything that has to do with incisions. I have passed out with suture removal in the past – not from pain – but from the idea of removing sutures. It is irrational, like a fear of needles but with incisions.
POST OP FOLLOW UP
On Wednesday morning I have my postop visit with my PA. It goes really well, everyone thinks my progress is amazing which is a relief because I just keep thinking of the 80 year old lady I spoke with who lived alone and was doing her own laundry on day 3 lol! I have been worried that I am not progressing as quickly as I should, but, just like my surgeon told me prior to surgery, this is a very invasive regardless of it being anterior. He told me there is a long recovery. He told me that I wouldn’t drive for 4 weeks. I did not believe him because of all of the people who’ve had this done who told me this would be easy and I’d be back to normal within a couple of weeks. I think hip replacement surgery must be like child birth, once you are recovered you completely forget any pain and discomfort.
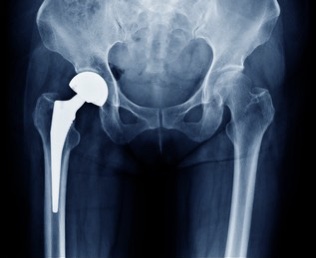
They took x-rays at this appointment and I was able to see my hip implant – that was pretty cool! I brought up my leg length discrepancy – although it has gotten so much better that I am not really worried about it. My PA did some measurements on my x-rays and assured me that if there is a difference, it is less than 1 mm which is the best that I could hope for. He tells me that my implant is the smallest they make without custom ordering one – a size 2. Who knew my hip implant would make me feel skinny? On the other hand, I am apparently small boned so there goes using being big boned as an excuse to be a little fluffy.
Upon looking at my bandage rash it was decided that I would start a 5 day cortisone pak, which will also work as an anti-inflammatory for my hip so I can stop taking the Ibuprofen. Even though the itching has thankfully stopped, it is still quite red and bumpy so I am thankful to have something to help this rash move on out. He removes the remaining portion of my steri-strip/tape and all is well with the incision. He says in about another week it is okay to start using polysporin or vitamin e oil for scarring.
I told him I was surprised at how much thigh and muscular pain this operation had caused and he said that was completely normal and that this is really a huge surgery. The “easy” part comes in comparison to what hip replacement looked like 15 years ago, where I would not even walk for days after surgery and would be required to go to inpatient rehab for several weeks. He also reminded me that I had only taken 1 Percocet. Good point. He says that in just a few weeks this hip will feel completely natural and I will be amazed. I choose to believe him. I will see the surgeon in 4 weeks and that will be it!
SUMMARY FIRST TWO WEEKS
My overall thoughts are that it has, in terms of a major surgery been easy. The pain has all been centered around my thigh and felt mostly muscular. I was thinking that this was worse than it should have been but based on my appointment today, apparently not. Prior to this surgery my abdominal CT scan showed “atrophy of the right gluteus minimus and medius” so its not like I went into this surgery with strong muscles on my right leg. I could feel the differences when doing yoga between the two sides – the right side would shake in positions and sometimes, I just couldn’t do them, while my left side had no issues at all.
For me this has been much tougher mentally than physically. I have had a ton of anxiety from the time I found out that I needed a hip replacement. Post operatively, not being able to walk, hike, and do yoga has really eliminated all of my coping mechanisms. I didn’t even drink any wine lol! It was hard to wrap my head around having a hip replacement at 53. My fifties have given me a lot of health issues that I didn’t ever expect to have to deal with, and certainly not this young (*ahem – relatively speaking). Life has been really challenging for me for a lot of years with things completely unrelated to my hip. Then, I had to have surgery in a Covid surge and the surgical center experience still bothers me to be honest. I tell you all of this because, other than enduring Covid protocols, the other things might be unique to me that factor in to my recovery and perception of it.
I cannot end my summary of this without saying that it was the kindness of my friends, my daughters, and most especially my husband that kept my spirits up and gave me a reason to be thankful every single day. Meals, flowers, cards, visits, phone calls and texts were so helpful and so important to me during this time. I hope my friend Linda has it correct, because I haven’t been hip in a very long time, I’ve been a grumpy old woman in pain.

week three
This week has been a turning point for sure. In all fairness, I think I have been helped immensely by the 5 day course of Prednisone I have been taking for that nasty allergic reaction the bandage caused, which also reduced any inflammation in my hip. But, as noted above, I would’ve been taking Celebrex for 30 days post op so I think the Prednisone just put me where I should be in terms of post surgical inflammation.
I really wanted to have a measurable source of movement and so I started doing the elliptical this week – no resistance whatsoever and at a very leisurely pace. I also drove around the neighborhood with my husband and received his stamp of approval to begin driving short distances this week.
My only sources of discomfort are sensation oriented and not really pain. The area where my incision is sometimes feels like it is burning. On the upside of that, I am starting to get feeling back on the side of my thigh, which I think is the reason that I occasionally get shooting nerve pain in my thigh. All of these things are weird but completely manageable. Since the surgery, when I lay down to sleep at night it feels like there is a stretching feeling in my groin and for the first 10 days or so I did sleep with my foot on pillow which alleviated that, but it has definitely improved this week to the point that I don’t really notice it anymore.
The other thing I’ve discovered this week is that I haven’t been walking properly for I don’t know how long. I am suddenly able to take longer strides and it feels amazing, but very unnatural at this point. I still have a limp, but it has only been 3 weeks so I’m not too worried.
I’ve started focusing on moisturizing my skin around the incision site – the skin is very dry and perhaps that is the source of some of the discomfort I feel. The rash outline where the bandage was is still there but definitely improving, I feel like moisturizing will only help that go away completely. I’m also lightly massing my thigh as there is some soreness still and I have numbness.
All in all, its been a great week and I’m hoping Week 4 comes with just as much progress.
week four
During this week, my limp improved substantially and I clocked a mile walking for the first time which kind of opened up my world.
I am able to lay on both sides of my body, but am afraid to fall asleep there for fear that I move the wrong way and dislocate my hip.
My hip joint is beginning to feel like a natural part of me, however, my thigh and incision are definitely not. I have crazy nerve discomforts in various different spots that randomly cause me pain. This is not constant and does not happen all the time, but the feeling ranges from electrical shots of pain to a burning sensation.
My incision is “healed” in that is closed, however, it is still lumpy for lack of a better word. It is improving, just at a snail’s pace. I have loss of sensation over the side of my thigh, but it is getting better and so I am hopeful that eventually my thigh will feel completely normal.
My movement in general is becoming much more natural and I only notice discomfort when bending over at the waist and also trying to lift my leg up with a bent knee – like when I am getting dressed or putting on socks or shoes. I can do all of these things without assistance, but not without some discomfort.
One thing I have been able to do this week that I couldn’t prior to the surgery is a straight leg lift when lying on my back. It is due to my yoga practice that I knew I couldn’t do this, and for some, this might not be something you ever do, or have any desire to do, but for me it was a significant issue. I couldn’t lift my extended, straight right leg even an inch off the ground prior to surgery, while my left one had no issue whatsoever. I’m happy to report that I can now lift my right leg as well!
I am still experiencing muscle soreness this week, and continue to be amazed that the real recovery of this surgery is not the metal implant in my hip, but the muscle and nerve recovery from having to go through these things by separating them to get to my hip joint. Again, some of this muscle soreness is due to the fact that my muscles were atrophied prior to surgery.
I stopped wearing the calf wraps that squeezed my calves while sleeping to prevent blood clots. I didn’t mind them too much, but it is nice to be done with them.
Wow Cathy, that’s alot to go through. I understand the anxiety. With far fewer problems I have been experiencing that too! And the rash…I so identify! I was on a 2 week heart monitor and have these rashy bumpy, almost bruised patches from the leads.
I have not been through the kind of surgery that you had, but it brings me comfort and perspective as I head to the doctor for other things. Hearing your story makes me feel a little less alone in navigating my Healthcare.
I’m sending you comforting, relaxing thoughts and hope you are feeling much more back to yourself soon.
LikeLiked by 1 person
Robin you are so sweet to read this very long post! ♥️ I hope that whatever health issues you are facing are not too serious and most importantly 100% resolvable. I’m sending you all my love and positive vibes as you navigate. This getting old stuff is for the birds! 😂
LikeLike
Thank you for taking the time to detail your early journey through your hip replacement. I’ve just finished week 3 of my recovery from the first (of both) anterior approach replacements. To my surprise, I think I’m glad I read your blog post after surgery. It’s too long a story for me to explain that comment, but it’s more about me than you. Primarily your post has reassured me that the nerve and muscle recovery is normal and expected. I hadn’t given it enough thought, but I’m working my way through things. My surgeon told me it takes about a year for your body to fully adjust to the new hip, so I’m guessing you’re just about at that point now. Congratulations. 😊👏
LikeLiked by 1 person
Hi Francine! I hope that you are improving daily – 3 weeks is definitely still in full recovery mode! I am almost 1 year and sometimes I forget I’ve had a hip replacement.
LikeLike